We’ve all heard that regular physical activity is important to your overall health and wellness. But why? Being active helps to improve your mood, clear your mind, minimize stress, provide more energy, build and maintain muscle, manage your weight and protect your heart.….just to name a few. The recommended amount of physical activity is 150 minutes per week that includes 2 days a week of muscle strengthening activities, also known as resistance training. Did you know that just 20 minutes of resistance training twice a week can lead to major improvements in body weight and blood sugar levels? Examples of these types of exercise include walking, biking, swimming, weight lifting, running, gardening, doing chores around the house and even being intimate.
For people managing Type 1 Diabetes, being physically active can get a little tricky at times. When you are active, your muscles use sugars that are either stored in your body or are floating around in your blood stream for energy like gas for a car. Certain types of exercise can lead to low blood sugars while other types of activity can lead to high blood sugars. It is important to understand how activity and exercise affects blood sugars so that you can plan ahead to stay safe and enjoy what you are doing! As you exercise more, your body may become more sensitive to insulin, increasing the risk of low blood sugars during physical activity or for up to 48 hours after. Finding the right balance with carbohydrates and insulin to manage blood sugars during and after activity can be a challenge. Your diabetes educators are here to help you!
Let’s review the three types of exercise:
- AEROBIC – light to moderate intensity exercise for more than 10 minutes.
Blood sugars tend to drop more often during and after aerobic exercise
e.g. cardio, running, swimming, biking, skating
- MIXED – alternating periods of moderate to high intensity exercise.
Blood sugars tend to stay the same, but you should still watch closely
e.g. basketball, soccer or high intensity interval training (HIIT)
- ANAEROBIC – high intensity resistance exercise.
Blood sugars may spike (go high) and you may need to correct after anaerobic exercise
e.g. weight training, resistance bands, cross-fit, jumping rope
Planning Ahead for Exercise
There are a few different ways you can prepare for exercise to help prevent low or high blood sugars.
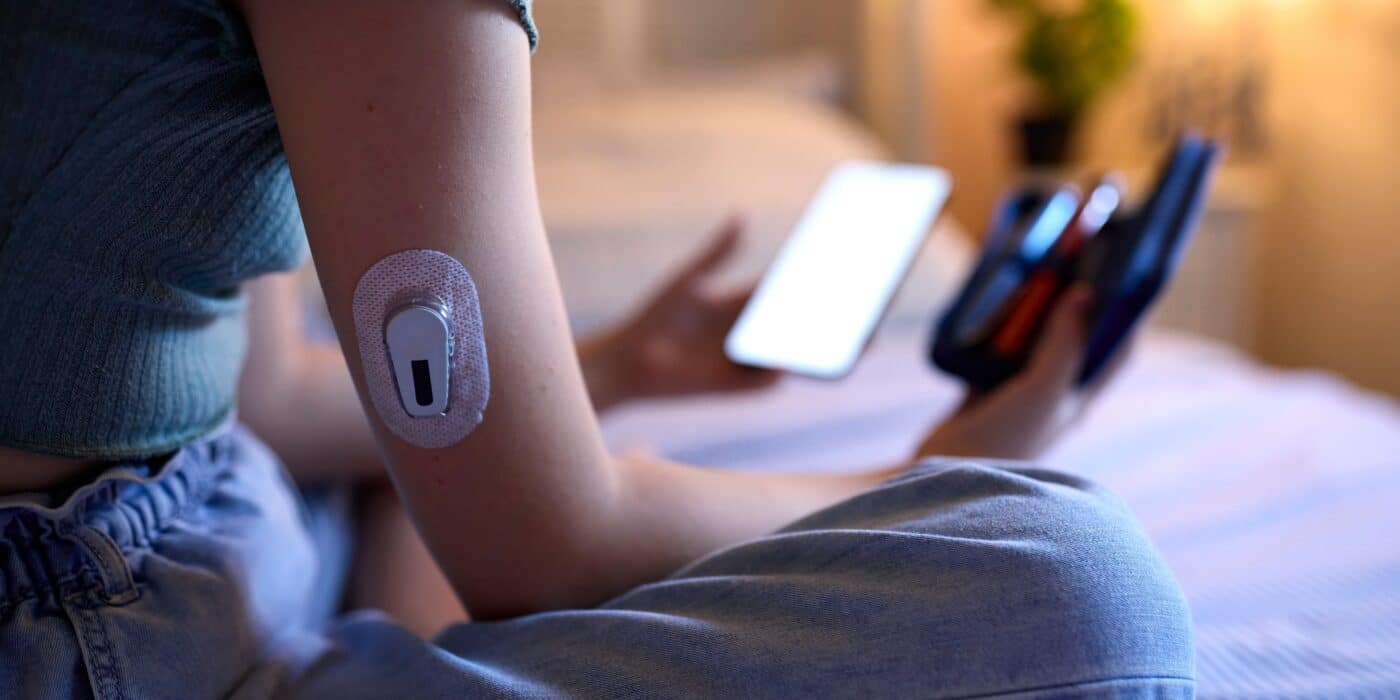
Consider using technology:
Take advantage of technology by wearing a continuous glucose monitor sensor that gives you quick access to your blood sugar readings. Use trend arrows to help make decisions about whether to have a snack or take a break from activity. If you do not wear a sensor, check your blood sugars more often with a finger poke while you are exercising and for the next 48 hours after. Set an alarm on your phone to check blood sugars around three o’clock in the morning; especially if you have a very active day.
Adjust insulin before or after exercise:
If you wear an insulin pump or manage your blood sugars with multiple daily injections (MDI), you may want to adjust your pre-meal bolus dose depending on how intense the activity will be, how long you will be active for, how much insulin you have on board (IOB) and when your last meal or bolus was taken. You may need to adjust your insulin up to 90 minutes before starting any activity.
If you are going to be active within two hours of your last meal, or your blood sugar reading is under 7.0mmol/L, you may want to eat 20-30 extra grams of carbs or take only half of your usual insulin dose. If you are wearing an insulin pump and plan to be active more than two hours after your last meal, you may want to run a temp basal rate for 90 minutes before you plan to start exercising. Set it to run during your activity and up to 1-2 hours after you are finished to help manage blood sugars. You may also want to consider setting a temp basal rate at bedtime to reduce your insulin by 10-20% to avoid having a low blood sugar through the night. Your needs may be different, especially as you exercise more or try different activities. Speak to your diabetes educator to find the right temp basal setting for you.
Be careful where you inject insulin before exercise:
Be sure not to inject insulin in or around muscles in your arms or legs before exercise. As muscles get warmed up, sensitivity to insulin increases, which means the risk of a low blood sugar also goes up if insulin is injected in areas that muscles are being used.
Consider ExCarbs:
Speak to your diabetes educator about another strategy you can used, called ExCarbs to help figure out how many grams of carbohydrates you should eat before, during and after your activity or how many units of insulin you should subtract from your usual pre-meal dose.
Stay Safe:
Plan your activities with a friend or loved one who knows how to recognize symptoms of a low blood sugar and what to do to help you if you have a low blood sugar. Make sure to wear medical alert identification and proper shoes that fit well. Do not exercise if you are not feeling well or have ketones.
Follow the GOLDEN RULE: make sure to ALWAYS carry low blood sugar treatment supplies like glucose tablets, juice boxes, regular pop or candies and drink extra water to stay hydrated. As a general guideline, you should drink water before starting activity and drink 250mL of water for every 20 minutes of exercise.
Watch and see how physical activity affects you!
It may take some time to learn what works best for you to manage your blood sugar when exercising. Try different kinds of activity or make changes to the intensity or amount of time you exercise until you find the right fit. Remember to check your blood sugars before, during and after activity to see how your body reacts to exercise. You may want to keep a journal to track and look back on what you have already tried and how well it works or what changes need to be made. Always speak with your healthcare team before starting a new activity for help adjusting your insulin or pump settings. Happy Exercising!
Join Diabetes Depot for the ‘Adjusting for Activity’ workshop on July 6th from 7:30 to 8:30pm ET for more information. Click the link to register: https://diabetesdepot.ca/index.php/workshops-ask-the-expert-sessions/
ADDITIONAL RESOURCES:
Diabetes Canada – Planning for Regular Physical Activity
https://www.diabetes.ca/diabetescanadawebsite/media/managing-my-diabetes/tools%20and%20resources/planning-for-physical-activity.pdf?ext=.pdf
Diabetes Canada Podcast – Diabetes 360 with Dr. Mike Riddell (Season 1, Episode 7)
https://blubrry.com/diabetes_canada_podcast/28940433/diabetes-360-season-1-episode-7/#autoplay